Table 1 summarizes BP targets for older adults across the four guidelines. For robust or mildly frail older individuals, JSH2025 and AHA/ACC 2025 recommend < 130/80 mmHg regardless of age (75, 80, or 85 years) [3, 4]. This intensive target in JSH2025 is explicitly supported by the guideline committee’s meta-analysis [5], which included landmark trials such as SPRINT [7, 8] and STEP [9] that demonstrated cardiovascular benefits of intensive BP control in older adults. In contrast, ESH2023 suggests 140–130 mmHg initially for those aged 65–79 years, with further reduction to <130 mmHg if well tolerated, and 140–150 mmHg for those ≥ 80 years [1]. ESC2024 proposes the most intensive target of 120–129/70–79 mmHg for patients < 85 years but recommends <140/90 mmHg for those ≥85 years or with moderate-to-severe frailty [2].
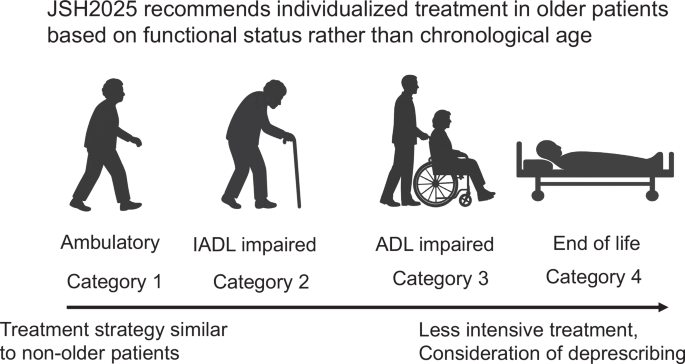
For functionally impaired older people, JSH2025 provides detailed, tiered recommendations based on its four categories [4]. Category 2 (impaired instrumental ADL) targets <140 mmHg, with <130 mmHg considered if tolerable. Category 3 (impaired basic ADL) aims for <150 mmHg. Category 4 (end-of-life) individualizes targets around 140–160 mmHg, explicitly addressing deprescribing considerations.
ESH2023 and ESC2024 also recommend individualized, more conservative targets for frail patients (140-150 mmHg and <140 mmHg, respectively) [1, 2], while AHA/ACC 2025 emphasizes shared decision-making without specifying numerical targets for frail populations [3].
The variation in BP targets reflects different interpretations of available evidence. ESC2024’s lower targets are influenced by recent trials such as STEP [9] and SPRINT [8, 9], which demonstrated cardiovascular benefits with intensive BP lowering. However, these trials predominantly enrolled relatively healthy older adults, with limited data on very frail or institutionalized individuals. JSH2025 acknowledges this evidence gap and adopts a pragmatic approach: intensive treatment for fit older adults (supported by the guideline committee’s systematic evidence synthesis [5]) while providing clear guidance for those with declining function, informed by observational studies such as PARTAGE [10], which suggested no benefit from intensive BP lowering in frail nursing home residents. Category 2 represents individuals with IADL impairment who remain able to attend outpatient care, whereas Category 3 reflects patients with more advanced disability, often comparable to nursing home residents. Evidence from the PARTAGE study, conducted in nursing home residents, does not define a precise upper SBP boundary [10]. Although no RCT directly supports a specific target for this group, setting <150 mmHg is consistent with data from HYVET [11] and with deprescribing evidence from OPTIMISE, both of which suggest that SBP levels around this range are safe in very old or frail populations [12]. For Category 2, evidence supporting permissive targets up to 150 mmHg is limited; therefore, JSH2025 recommends < 140 mmHg, considering < 130 mmHg if tolerated.
JSH2025’s detailed categorization offers practical advantages in clinical settings. By explicitly linking functional status to BP targets and treatment modifications, it reduces clinical uncertainty and supports consistent decision-making across diverse healthcare providers. Furthermore, JSH2025 addresses end-of-life care (Category 4) more explicitly than other guidelines, recommending consideration of gradual dose reduction or discontinuation of antihypertensives in terminally ill patients—a reflection of Japan’s cultural emphasis on quality of life and dignity in end-of-life care.
Another unique aspect of JSH2025 is its recommendation to initiate antihypertensive medications at half the standard dose for individuals ≥ 75 years or those aged 65–74 with significant functional decline, with gradual titration while monitoring for adverse effects. This cautious approach contrasts with ESC2024’s preference for starting with long-acting dihydropyridine calcium channel blockers or renin-angiotensin system inhibitors, and ESH2023’s suggestion of monotherapy in frail patients with grade 1 hypertension.
link




More Stories
Do No Harm: Rethinking Diabetes, Hypertension in Frail Older Adults
Women with pre-pregnancy high blood pressure face breastfeeding challenges, Ohio University study suggests
New high blood pressure guideline emphasizes prevention, early treatment to reduce CVD risk