Patient characteristics
We included a total of 393,495 adult patients admitted with LGIB. Of these, 31,565 (8.02%) were transferred from another acute care hospital, while 361,930 (91.98%) were directly admitted to the hospitals (Fig. 1). Table 1 shows the characteristics of the patients and the hospitals in which they were treated. We found that transferred patients, when compared to non-transferred ones, were younger (66.39 vs. 67.23 years, P < 0.01), more likely to be males (52.51% vs. 47.59%, P < 0.01), and had higher (≥ 3) CCI scores (40.86% vs. 38.64%, P < 0.01). From the hospital standpoint, transferred patients were more often admitted to large-sized (62.63% vs. 48.19%, P < 0.01), teaching hospitals (84.65% vs. 71.80%, P < 0.01) located in urban areas (95.09% vs. 92.93%, P < 0.01). Table 2 shows the prevalence of different comorbidities in our target cohort.
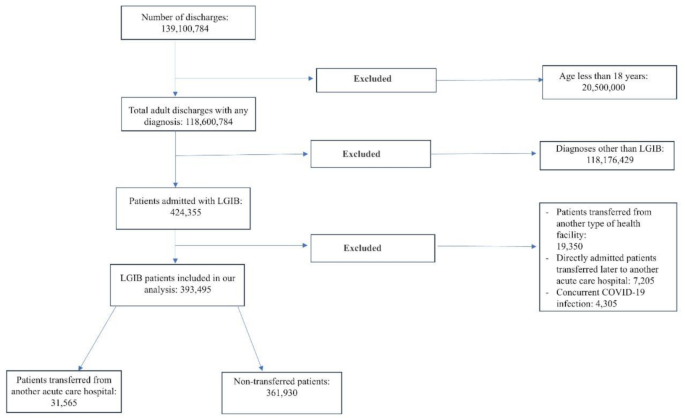
Flow diagram depicting the inclusion and exclusion of patients with LGIB
We devised a surrogate LGIB severity score, using diagnostic codes for individual components of Oakland score criteria (Table 3). The severity score was calculated by adding points assigned to each component, as defined by the Oakland score criteria [15]. Patients transferred from another acute care hospital had higher mean severity score than those who were admitted directly (8.35 vs. 7.06, P < 0.01).
Mortality and morbidity
LGIB patients who were transferred from another hospital had higher odds of inpatient mortality (adjusted odds ratio (AOR) 1.96, 95% CI (confidence interval) 1.77–2.18, P < 0.01) (Table 4). We found that transferred patients had higher adjusted odds of acute kidney injury (AKI) (AOR 1.37, 95% CI 1.28–1.45, P < 0.01), AKI requiring dialysis (AOR 2.41, 95% CI 2.07–2.83, P < 0.01), septic shock (AOR 2.11, 95% CI 1.91–2.34, P < 0.01), mechanical ventilation (AOR 2.63, 95% CI 2.39–2.88, P < 0.01), and intensive care unit (ICU) admission (defined by need for vasopressors or mechanical ventilation, with either indicating ICU admission) (AOR 2.61, 95% CI 2.39–2.86, P < 0.01).
Analysis of major adverse cardiac and cerebrovascular events (MACCE) revealed that patients transferred from another acute care hospital had elevated odds of acute heart failure (AOR 1.23, 95% CI 1.11–1.35, P < 0.01), acute myocardial infarction (AOR 2.20, 95% CI 1.87–2.58, P < 0.01), ventricular arrhythmias (AOR 1.58, 95% CI 1.36–1.83, P < 0.01), and acute transient ischemic attack/stroke (AOR 2.69, 95% CI 2.29–3.17, P < 0.01) (Table 4).
Procedural performance
We found that transferred patients had slightly higher rates of diagnostic CSP (AOR 1.11, 95% CI 1.03–1.20, P < 0.01) but lower odds of CSP with intervention (AOR 0.85, 95% CI 0.79–0.92, P < 0.01) and repeat colonoscopy (AOR 0.84, 95% CI 0.75–0.94, P < 0.01). There was no difference in the total number of colonoscopies performed among the two cohorts (AOR 0.96, 95% CI 0.90–1.02, P = 0.17). Furthermore, the transferred patients had significantly elevated odds of undergoing IR-guided embolization (AOR 2.68, 95% CI 1.93–3.74, P < 0.01) (Fig. 2). Further analysis revealed that the mean duration between the initial presentation to the final intervention (CSP or IR-guided embolization) was shorter in transferred patients (3.34 vs. 4.97 days, P < 0.01).
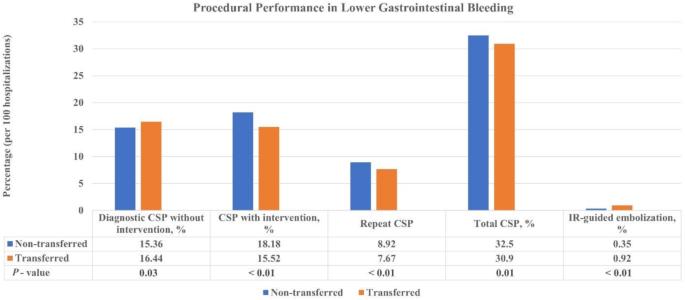
Procedural performance in LGIB among transferred and non-transferred patients
Resource utilization
From a resource utilization viewpoint, transferred patients had an increased mean LOS by 4.37 days (Absolute percent difference (APD) 1.56, 95% CI 1.51–1.62, P < 0.01) and higher total hospitalization charges by a mean of $61,239 (APD 1.65, 95% CI 1.56–1.75, P < 0.01) (Table 3). Additionally, a higher proportion of transferred patients were discharged to rehabilitation facilities compared to their non-transferred counterparts (AOR 1.52, 95% 1.42–1.63, P < 0.01).
link





More Stories
Pediatric Gastroenterology – MU Health Care
Leading Gastroenterology Hospitals Advancing Digestive Care in India
Mobile ‘Endoscopy on Wheels’ Delivers Lifesaving Gastrointestinal Care